Transgender (F-M) Mastectomies (“top surgery”)
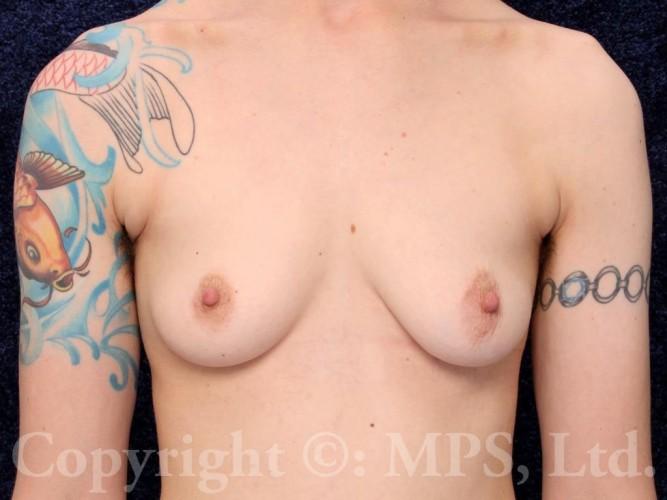
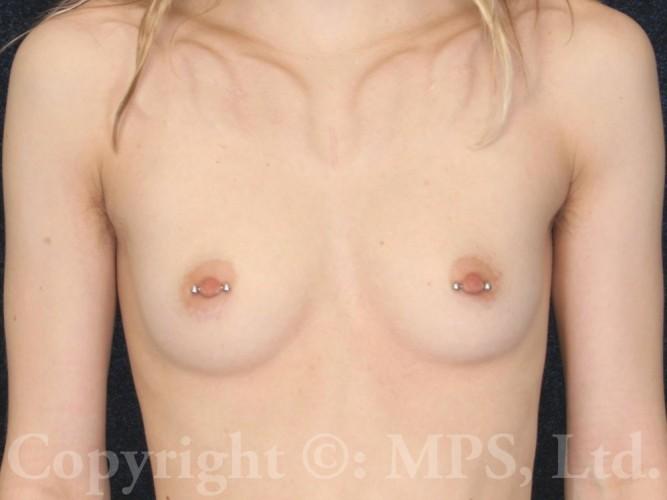
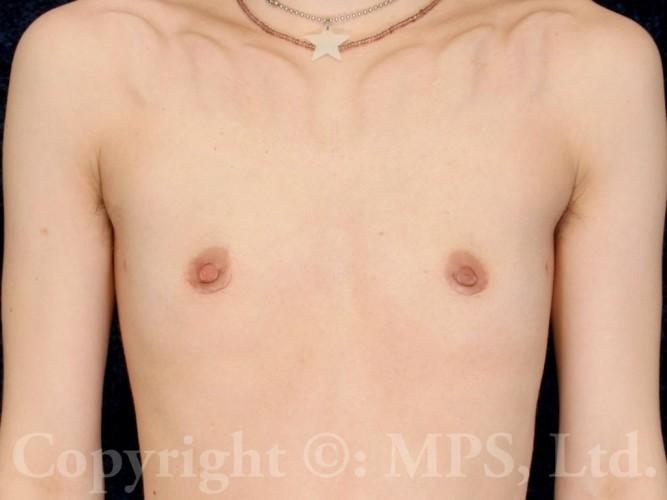
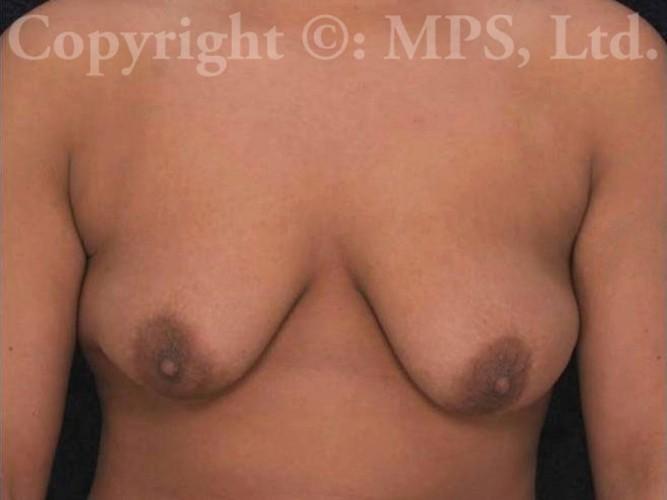
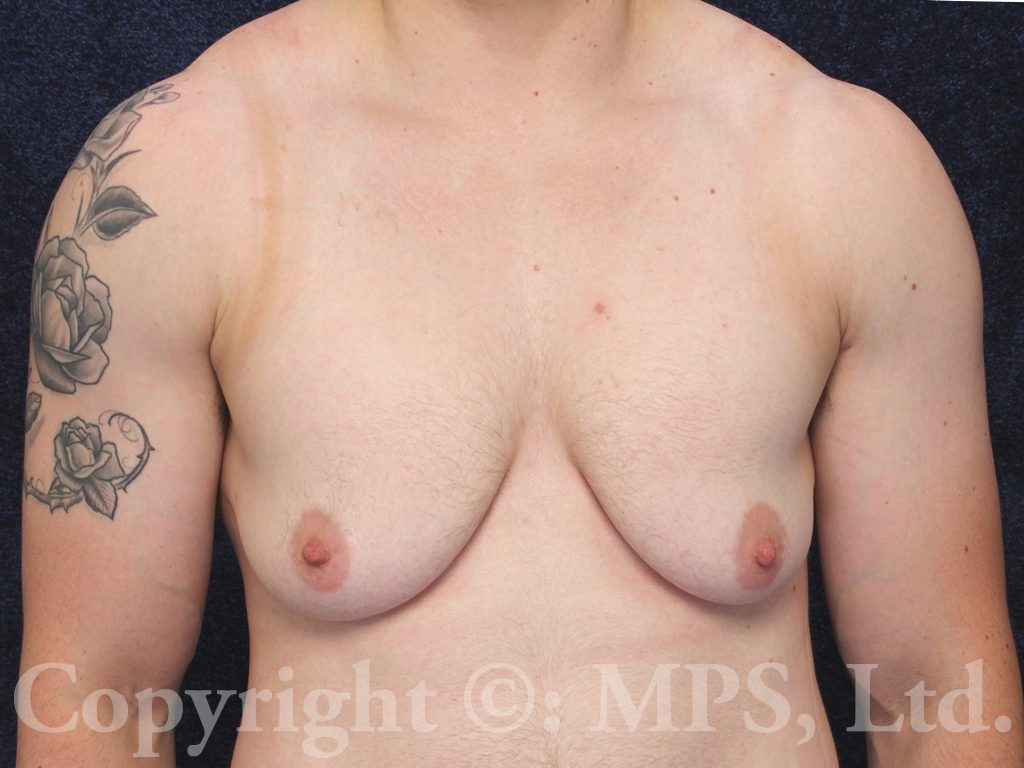
F-M transgender patients may request breast removal (transgender mastectomy, or “top surgery”) as the first and sometimes only surgical step in their gender reassignment process. Depending on the size of the breasts, as well as the elasticity and tone of the breast skin, various procedures are available to create a masculine chest appearance. Testosterone therapy will not cause meaningful breast size reduction in the majority of transmen, nor is it necessary to be on Testosterone (though certainly safe and appropriate) for patients requesting mastectomies and a masculine chest appearance. (text continues after photos)
WARNING:
This gallery contains nudity not suitable for those under 18 years of age. By viewing you acknowledge this warning
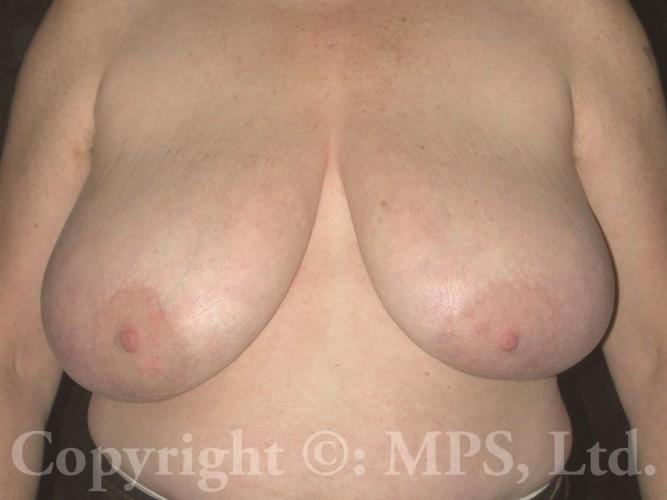
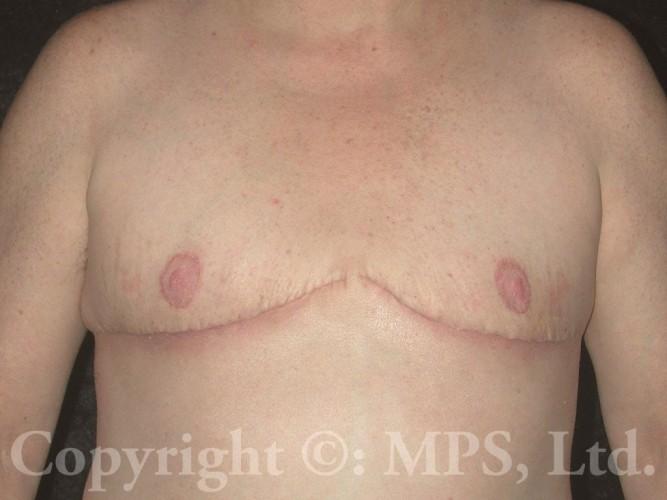
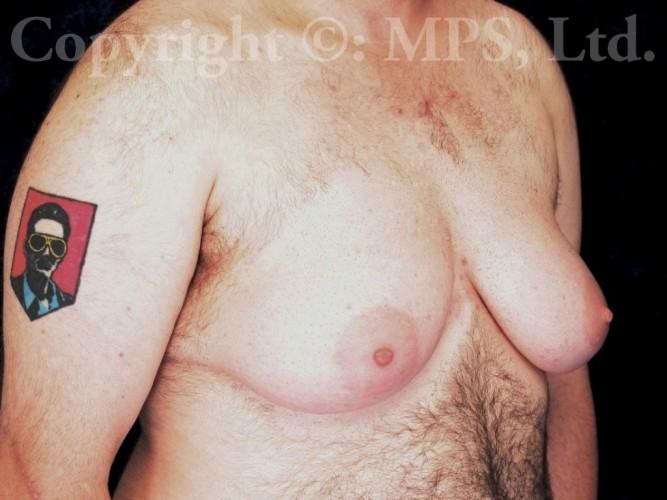
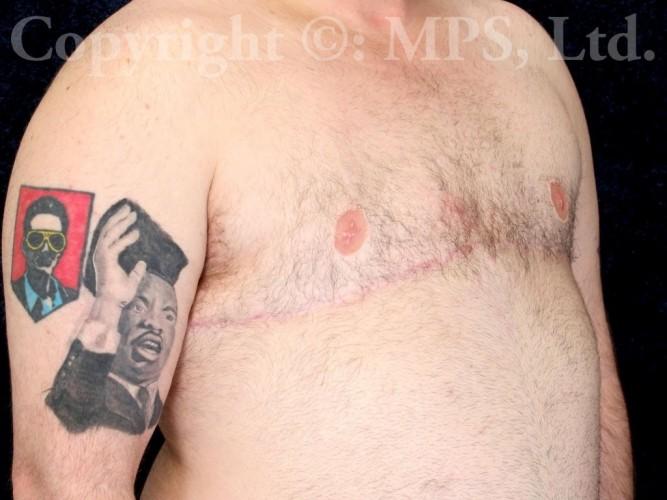
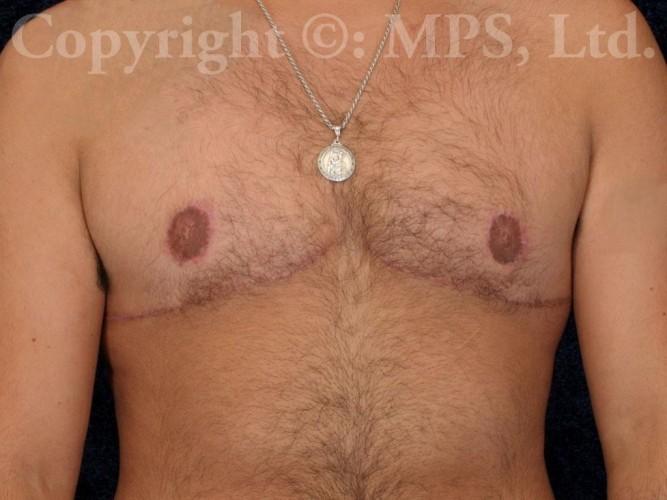
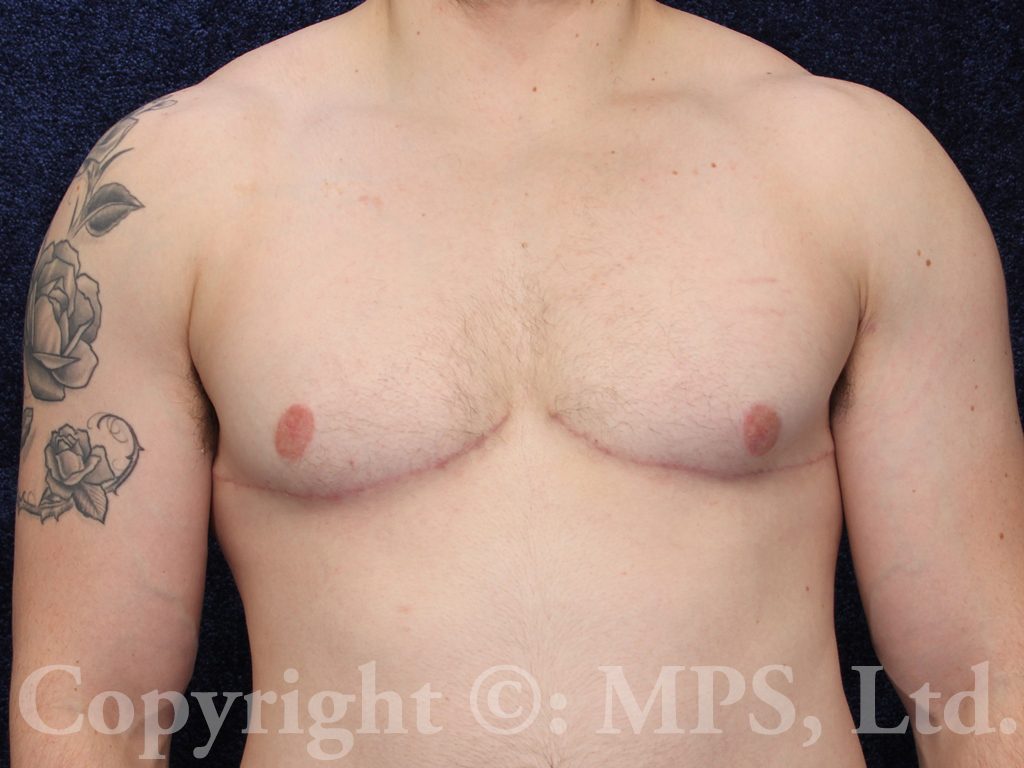
For all but the smallest breasts, the most common operation involves bilateral total mastectomies with excess breast skin removal with grafting and reduction of the nipple/areola complexes; this procedure is needed when transmen have both excess skin and breast tissue. This is commonly called the “double incision,” “elliptical excision,” or “skin-reducing” technique. Performing “keyhole” mastectomies when skin-reducing mastectomies are necessary is a huge mistake–loose, wrinkled skin, and a “caved-in” chest is NOT preferable to well-positioned and skillfully sutured incisions. (Search “bad top surgery” for some examples of what I am describing.)
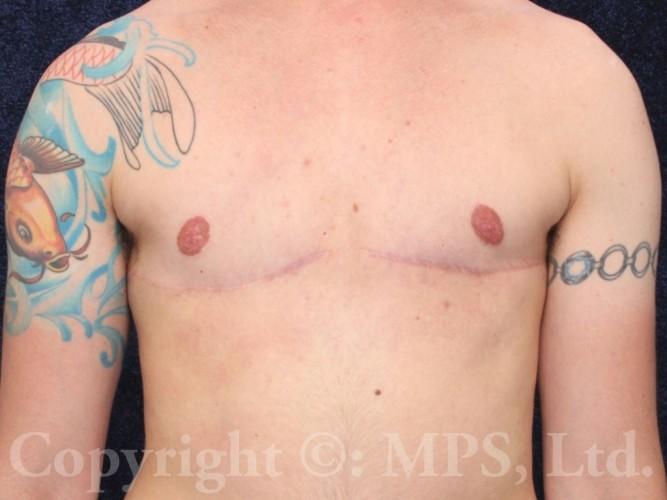
A well-performed top surgery procedure leaves scars on each side of the chest, and skillful incision placement (avoiding female breast reduction scar patterns) can help the final faded scar to be positioned along the lower edge of the pectoralis major folds, simulating normal male anatomic features while making the scars less apparent. Careful measurement and precise skin closure in layers avoids the vertical scars of female breast reduction operations. Plastic surgeons who use “standard” female mastectomy or breast reduction techniques will leave scars that are both unnecessary and unsatisfactory–ask to see photographs of actual patients like we have in our photo gallery.
Hair growth in patients on testosterone therapy can further conceal scars. In most cases (nipple grafts are not chosen by some patients), both nipples and areolas are reduced in size and placed as free grafts in the appropriate male position on the chest. Comparing female anatomy to male anatomy will show that male nipple placement is lower and lateral, near the edge of the pectoralis muscles, not more central and medial as in women. Proper positioning is critical to obtaining a masculine-appearing chest. Specialized dressings are used on each nipple/areola graft until the first bandage change; a drain is placed in each mastectomy space beneath the skin flaps to facilitate healing. Both graft dressings and drains are usually removed at 7-10 days post-op, depending on the amount of drainage. Both the mastectomy scars and nipple/areola grafts must be kept dry and protected from excessive activity or shear forces for a total of three-four weeks in order to reduce bleeding, bruising, seroma formation, and failure of part or all of the nipple grafts to “take” and heal properly to their recipient areas. Absolute avoidance of tobacco (nicotine) products including vaping, nicotine gum, patch, spray, etc., and even exposure to second-hand smoke is critical to skin graft healing. Scars are permanent, but will fade over 6-12 months; ultraviolet exposure must also be avoided during this period when scars are still pink and susceptible to hyperpigmentation.
Patients who are obese or have large, pendulous breasts may also require chest liposuction or additional skin tailoring (“dog-ear” excision) for optimal results; every effort is made to reduce the need for secondary surgery for any reason, though optimal results may require lateral chest or other revisions, often possible via local anesthesia.
In F-M transgender patients with small breasts and small areolas, minimal excess skin, and no skin laxity (sag or droop), a periareolar or “keyhole” mastectomy may be possible; the entire breast is removed through a small incision made at the junction of the darker areolar skin with the adjacent lighter skin. This avoids the longer scars of the skin-reducing mastectomies described above, but the areolar diameter is unchanged and may not be in the normal male orientation on the chest wall. Nipple size and protrusion can be reduced as needed or desired with keyhole mastectomies, but sensation to the nipple area is usually lost with both keyhole and skin-reducing operations. Surgeons who claim to preserve nipple sensation may not be removing all of the breast tissue, and in our opinion this retains risk of developing breast cancer as well as leaving undesirable contours. Using female skin incision patterns in transgender top surgery, or “leaving some tissue to preserve sensation” shows lack of experience with this procedure, in our opinion, and should be avoided.
Discomfort after transgender mastectomies is mild to moderate and will be decreased by use of anti-inflammatory medications, muscle relaxants, and prescription pain medications. Most patients carry out normal everyday activities (non-strenuous) in a day or two after this outpatient operation; exercise or vigorous activity is absolutely prohibited for 4-6 weeks in order for the mastectomy flaps to heal, the nipple/areola grafts (if needed) to “take,” and to avoid bleeding or seroma formation requiring re-operation. As noted earlier, absolute avoidance of smoking, vaping (with nicotine), tobacco use of any kind, or nicotine (gum, patches, e-cigarettes, or spray) is critical to allow the nipple grafts to survive; this requirement includes avoiding even one cigarette or exposure to second-hand smoke. Weightlifting can be resumed in 4-6 weeks depending on healing.
It is important to understand that creation of a proper masculine appearance for transmen involves much more than “standard” mastectomies (as for cancer patients), breast reduction incision patterns (anchor), or even some gynecomastia operations. Typically the higher, more centrally-placed female nipple areola position is absolutely wrong for a true masculine appearance. Lower, more lateral placement is required, and the American Board of Plastic Surgery-certified plastic surgeons at Minneapolis Plastic Surgery continue to perfect transgender mastectomy techniques to create masculine chests for transmen requesting mastectomies. Individuals requesting mastectomies without nipple grafts will decrease both costs and avoid the healing restrictions needed when grafts are used.
Cost for Transgender Mastectomy (“top surgery”)
Skin-reducing F-M mastectomies, star-pattern nipple reduction, areola reduction, and nipple/areola reconstruction as full-thickness skin grafts requires 3 ½ to 4 ½ hours as an outpatient operation, and total cost for a 4-hour average is approximately $16000. “Keyhole” or periareolar mastectomies may or may not require nipple reduction, and will take less operative time; average costs for this procedure are around $12000. Skin-reducing double incision mastectomies without nipple/areola grafts will be between these, based on surgical time estimates. Exact cost quotes are always available at the time of complimentary consultation with our American Board of Plastic Surgery-certified plastic surgeons. Financing options are available. Please contact us for a no-obligation consultation with one of our plastic surgeons and our kind and caring staff.
Insurance coverage for top surgery patients has not been common, despite many insurance companies claiming they will provide benefits for transgender patients. They then either fail to approve coverage or place restrictive “guidelines” to fulfill criteria. This is especially true for under-18 transgender patients. We are happy to consider top surgery for all transmen seeking state-of-the-art top surgery in an understanding and welcoming environment.
Because of the high demand for free consultations with our plastic surgeons, our staff will ask for a credit card number in order to schedule a consultation; there is no charge whatsoever for appointments that are kept–you will be charged $100 only if you fail to keep a scheduled appointment, or fail to cancel at least 48 hours in advance of your appointment time–for Monday appointments, you must cancel no later than noon on the previous Thursday; for Tuesday appointments, you must cancel by noon on the previous Friday.